Declarations:
Ethical Considerations:
The project was reviewed and determined to be exempt from full Institutional Review Board (IRB) review by the University of Alabama at Birmingham IRB.(No. IRB-300009210).
Consent for Publication:
All authors consent for publication.
Availability of Data Statement:
Data are available upon reasonable request to corresponding author.
Competing Interests:
All authors declare that we have no competing interests.
Funding:
This project is supported by the Health Resources and Services Administration (HRSA) of the U.S. Department of Health and Human Services (HHS) as part of an award totaling $2,278,815. The contents are those of the author(s) and do not necessarily represent the official views of, nor an endorsement, by HRSA, HHS, or the U.S. Government.
Authors’ Contributions:
JW and JC: Literature search, manuscript outline, design, preparation, and writing of the abstract, background, writing of methods (design), Strategies Used to Improve WE CARE Nursing Survey Response, discussion, limitation sections, conclusion sections, and creation of the table S.H and KM: Editing, interpretation of data results A.M: Data collection, writing of Survey Instrument, Data analysis write-up and results, and figure creation PP : Conceptualizing/refining the paper idea, writing Methods (The Program) section, manuscript revisions, final approval, final editing JW, JC, CB, JT, DM, and TB: Study implementation, and editing with grammatical corrections All authors reviewed and approved the manuscript
Abstract
Targeted interventions were implemented to address challenges with participation in a web-based survey administered semi-annually to nursing personnel at a large academic medical center in the southeast US. Intervention examples included face-to-face rounding, electronic links, and other incentives to address barriers like time constraints, survey fatigue, and respondent concerns with anonymity. These combined efforts resulted in a 146% increase in response rate between our baseline survey in June 2021 and January 2023. Elevating staff voices fosters collaboration, engagement, and continuous improvement in patient care quality and staff satisfaction.
Background
Low survey response rates among healthcare workers can be attributed to a myriad of factors, including time constraints due to demanding work schedules, survey fatigue due to the abundance of survey requests, a perceived lack of anonymity for respondents, and limited recognition of immediate benefits [5]. However, increasing survey participation is critical to adequately representing the voice of the healthcare workforce and obtaining representative data. The need for high-quality data to inform organizational decision-making, improve patient outcomes, and foster staff engagement and satisfaction underscores the urgency for strategic interventions to enhance survey participation levels. The purpose of this paper is to describe the success of our strategies in improving nurse participation in the organization’s nursing surveys.
Methods
Setting
This project was completed at a large academic medical center in the southeastern United States. Participants included staff nurses working on the various inpatient nursing units within the organization.
Design
Longitudinal data was collected via survey to assess the effectiveness of interventions aimed at increasing staff nurse response rates in a survey administered semi-annually to nursing employees. The project aim was to evaluate a series of strategies designed to increase nurse survey participation over a two-year period of time. The surveys were created and distributed through the QualtricsTM electronic survey system platform. Surveys were accessible for approximately 30 days.
In 2021, surveys were distributed via email with a written invitation and a hyperlink. Building upon this foundation, subsequent years saw the introduction of additional engagement tactics. Throughout the first two-years of the WE CARE project intervention we employed various strategies to harness and enhance survey engagement. In 2022, alongside the email distribution, the WE CARE team at the medical center, initiated routine “WE CARE rounds” on day and night shifts on every inpatient unit. This fostered face-to-face interactions with frontline staff, as well as staff support and wellness breaks with snacks, candy, stickers, and games that were available on the WE CARE cart. These rounds provided an opportunity to build relationships with the staff and distribute small appreciation incentives. During survey periods, these WE CARE rounds helped to encourage survey participation. Weekly survey participation reports were provided to nursing leaders to highlight accomplishments.
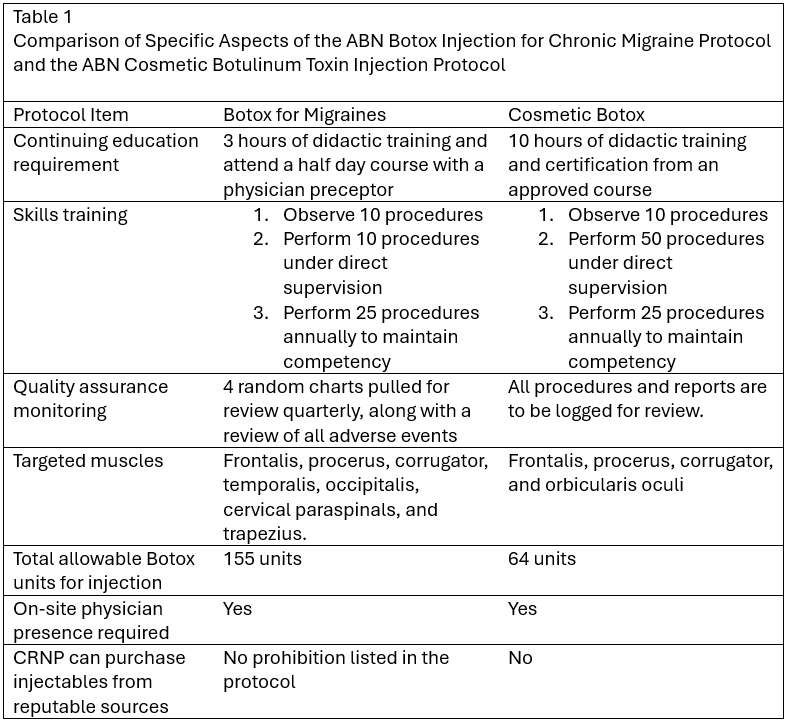
By 2023, the survey strategy expanded to incorporate more diverse approaches. In addition to the email invitations, unit rounds, and incentives, the team introduced QR codes and iPads (see Table). To ensure convenience and accessibility, the QR Codes were strategically placed around the unit workspaces for easy access to the survey—on computer terminals, in restrooms, and even by the time clocks. The QR codes allowed nurses to quickly access the survey via the camera app on cellular devices. Finally, iPads without employee login identifiers were available so staff could complete surveys anonymously. Personal identifiers were limited in the survey design to safeguard respondents’ anonymity and foster an environment of trust. Additionally, the project team emphasized the confidential and non-punitive nature of the survey. Furthermore, to maximize participation, all members of nursing services were encouraged to take the survey, regardless of their specific roles or positions.
The WE CARE team utilized “talking points” to inform the staff of tangible progress achieved and ongoing initiatives stemming from the invaluable insights gleaned from prior survey responses. Providing concrete examples of how the previous survey data were used to implement positive changes demonstrated the value of survey participation. Marketing flyers with survey dates were disseminated directly to unit nurse managers (NM) and NPDSs as a proactive approach to cascade information down to frontline staff. The active advocacy and endorsement of the survey initiative by NMs and NPDSs played pivotal roles in galvanizing staff nurse participation. Weekly reminders and updates were included during leadership meetings of the Chief Nursing Officer (CNO), Associate Chief Nursing Officers (ACNO), Associate Vice President of Nursing Value, Senior Directors of Nursing, Directors of Nursing, NMs, and NPDSs to complement these efforts. These updates highlighted the importance of the survey and reaffirmed the ongoing support of organizational leadership.
Data Analyses
Four-timepoints of data were downloaded from QualtricsXM and uploaded to Microsoft Excel. The responses were separated by role. Here, we were interested in capturing inpatient staff nurse information. The response numbers were counted using the recorded dates that were autogenerated by QualtricsXM. The recorded dates were further assessed by the number of responses by day. Graphical representations were created using Excel to show trends in the percentages of total responses by recorded dates for each survey time point (a total of four line charts) (see Figure).
Results
A total of 390 staff nurses participated in the baseline survey in June 2021. In June 2022, staff nurse participation increased to 808 nurse respondents—a 107% increase. In January 2023 there were 961 staff nurse participants, marking a 146% increase from the baseline of 390 participants. There was a decrease in July 2023 to 744 participants (23% reduction) compared to January 2023; however, this represented a 91% increase compared to the original survey in 2021. Although we had planned to administer the WE CARE nurse surveys over a period of 30 days, our graphs revealed that the surveys were left open for varied time periods: June 2021 – 33 days; June 2022 - 37 days; January 2023- 36 days; July 2023 – 33 days. The extra days were added to attempt to capture maximum participation, however, only in June 2022 did the extra days account for a large number of additional responses, as explained in Limitations below.
Discussion
To increase staff nurse survey participation, the WE CARE team implemented a multifaceted approach which included unit rounding, talking points, QR Codes, and iPads to enhance convenience and provide many communication channels for survey marketing and updates. This concerted effort mitigated privacy concerns and created a more efficient and effective process for survey completion. The change in survey participation from 390 to 961 staff nurses suggests the effectiveness of the implemented strategies, which resulted in larger response numbers and potentially more representative feedback from the bedside staff nurse workforce. Research studies consistently show that larger sample sizes yield more reliable and valid results [5, 6]. Even though participation decreased during the last survey time period, it was still significantly higher than at baseline. This decrease may have been result of survey fatigue due to the 6-month intervals between re-surveying. The devised strategies were a successful attempt to address the barriers to participation encountered by nurses, particularly the bedside staff nurses. Time constraints and survey fatigue are common challenges in healthcare settings [5]. The project navigated these barriers through the execution of unit rounds, provision of incentives, and integration of accessible technologies such as conveniently located QR Codes and iPads. Studies have indicated that addressing these barriers can substantially enhance survey response rates [9].
The year-to-year increase in the number of survey participants demonstrates the value of our simple but effective approach to obtaining nurse insight through survey participation. By proactively implementing measures to bolster survey response rates, nursing leaders can capture valuable insights, identify areas for improvement, and enhance the overall quality of patient care. Leadership engagement and support are pivotal in promoting survey participation [10]. The proactive engagement of NMs and NPDSs and consistent leadership reminders underscore the organization’s dedication to staff engagement. Research has shown a direct link between staff engagement and improved outcomes [22]. By identifying areas for improvement through surveys, healthcare organizations can implement targeted interventions, ultimately enhancing the quality of care provided to patients. Having the WE CARE team report back to front line nurses the actions taken by nurse leaders to address concerns revealed in prior surveys was yet another way to let staff know that their voice does indeed matter.
Research suggests that visible support and encouragement from leadership positively influence employees’ willingness to participate in surveys [1]. Ensuring anonymity and building trust are essential for honest responses [23]. By limiting personal identifiers, providing iPads, and emphasizing anonymity and non-punitive, the team attempted to create a secure environment. Using iPads enhanced participation and addressed concerns about anonymity, especially for individuals worried about maintaining privacy, without being logged on to a computer with their credentials or having to take the survey from their personal devices. Studies have shown that anonymous surveys yield more candid responses, more accurately reflecting employees’ opinions and experiences [2].
Potential challenges in sustaining the strategies implemented include budget constraints, evolving technology, and changing staff dynamics. Research indicates that long-term sustainability requires continuous adaptation and monitoring of survey methods [24]. In addition to survey fatigue among respondents, there is a potential risk of response fatigue among leaders who must frequently react to the findings. Balancing anonymity with analytic concerns represents another challenge. By conducting an anonymous survey there is a great opportunity for increased psychological safety that allows respondents to feel more comfortable disclosing sensitive information. However, on the downside, it reduces the ability to align results with specific demographic factors or to conduct true longitudinal analyses of respondents over time.
Limitations
Conclusions
Elevating the voice of nurses is vital for fostering a culture of collaboration, engagement, and continuous improvement in healthcare organizations. By implementing strategies to increase survey response rates, healthcare institutions can capture valuable insights, identify areas for improvement, and enhance the overall quality of patient care. Through transparent communication, simplified surveys, confidentiality, face-to-face marketing, incentives, and leadership engagement, healthcare organizations can create an environment where frontline staff feel empowered to share their experiences, ultimately improving patient outcomes and staff satisfaction.